“You gave me my life back!” One patient with Parkinson’s Disease expressed their gratitude to the nurse practitioner on a neurosurgery team after receiving Deep Brain Stimulation (DBS).
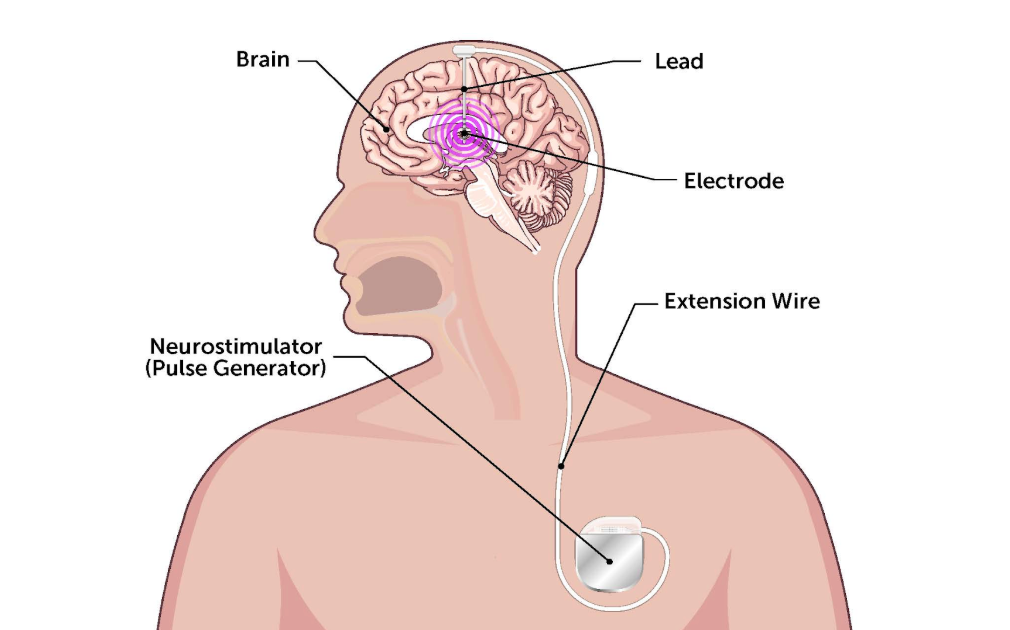
The three-part surgical procedure involves placing two leads (electrodes) in the brain that connect to a battery in the chest through extension wires. The electrical stimulation from the electrodes helps alleviate tremors, stiffness, slowness and dyskinesia. I learned this while shadowing Meredith Spadaccia, a nurse practitioner, for six weeks as a Summer Volunteer at Mount Sinai West Hospital. Patients come to get this surgery when medication alone is no longer able to manage their Parkinson’s symptoms.
However, many people are reluctant to undergo DBS as there are certain risks. They worry about strokes, even though the risk is only around one percent, according to a major university hospital report. There are also psychological hurdles. “There is misinformation on the internet about the procedure causing personality changes,” said Meredith Spadaccia.
Additionally, “Something unique with Parkinson’s patients is that you’re working with people who have impaired levels of dopamine,” explained Spadaccia. Dopamine is a neurotransmitter that gives you feelings of satisfaction and motivation. It’s much harder for these patients to feel the dopamine boost that encourages risk-taking. To help patients overcome this mental obstacle, “we remind them of how frequently DBS is performed, and how it has been around for decades. It’s about normalizing the situation.”
After the DBS hardware (electrodes, lead and battery) is fully set up, patients receive custom programming to optimize their symptom management. During programming sessions, the amplitude, frequency and pulse width of the electrical stimulation are adjusted to target specific Parkinson’s symptoms unique to every patient. This process often requires multiple visits over several weeks to determine the best settings for a given patient.
When programmed effectively, Spadaccia’s team helps patients balance their daily medication intake. She explained, “A few weeks after surgery’s done, we try to reduce medication by slowly titrating down.” Decreasing dosages and frequency might not seem impactful, but not having to take pills every two hours to manage symptoms can improve quality of life.
Spadaccia often recalls heartwarming moments that remind her why she chose this profession in the first place. Her grandfather had Parkinson’s, and seeing him suffer made her want to care for others. “You don’t often get to hear ‘You gave me my life back.’” There is currently no cure for Parkinson’s disease, but as Deep Brain Stimulation technology evolves, it offers many patients a second chance at life.