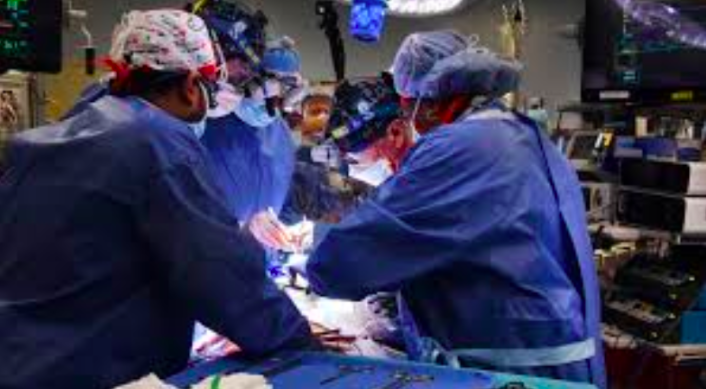
Courtesy of The New York Times
The nationwide organ shortage in America is pushing doctors to find new forms of life-saving medicine; one solution is Xenotransplantation, the transplantation of live cells, organs, or tissue from a nonhuman species to a human. Xenotransplantation can offer transplants when human materials are not available, which is even more important given the extensively long and expensive donor waiting lists for patients, prolonging their stay in ICUs and even loss of life. In particular, these transplants can be life-saving for conditions such as neurodegenerative disorders, chronic obstructive pulmonary disease, cardiomyopathy, liver cirrhosis, polycystic kidney and many more.
While xenotransplantation is a new form of surgery, the history of transplants goes back to 1933 when the first reported kidney transplantation took place in the Soviet Union. It was not until over 20 years later that this first successful transplant occurred, in 1954 between two identical twins. The organ matching system was created in 1977 by the Southeast Organ Procurement Foundation (SEOPF). This computer based system allowed organs to be transported to other hospitals and parts of the country if there was not a match at the original location. Up until the 1980’s, the quantity of transplants performed were greatly impacted by the high chances of organ rejection. This is one of the many issues that has occurred throughout the lifetime of transplants, which remains the highest risk in transplants to this day. This issue has been greatly improved in recent years with the help of immunosuppressive drugs. One of the biggest issues resulting from xenotransplantation is the risk of diseases spreading from the germs of a non-human being. Dr. Montgomery mentioned that infectious disease screenings are crucial for the progression of these transplants. Dr. Montgomery indicates that more sensitive screening for the donor pigs is important in order for the patient to have a higher chance of long-term survival.
Image from RGA
Xenotransplants are still being heavily researched and tested by doctors around the country, but in the past few years the field has seen multiple breakthroughs. On September 25, 2021, Dr. Robert Montgomery at NYU Langone, led two surgeries on cadavers. This innovative procedure offered lots of insight for doctors, and led to two more surgeries at NYU Langone in 2022, on June 16th and July 6th. These two procedures were conducted on two recently deceased patients, both performed over multiple hours. Genetic modifications are made to the pig heart to lower the risk of immune system rejection. There were no signs of rejection from the human bodies, and normal function was observed with the use of routine post-transplantation medications. Nader Moazami, surgical director of heart transplantation at NYU Langone was the leading surgeon on these cases.
Dr. Moazami said, “Our goal is to integrate the practices used in a typical, everyday heart transplant, only with a nonhuman organ that will function normally without additional aid from untested devices or medicines…We seek to confirm that clinical trials can move ahead using this new supply of organs with the tried-and-true transplant practices we have perfected at the NYU Langone Transplant Institute.” Before the past year, these types of research-based surgical procedures had only been performed on nonhuman species. This breakthrough will allow researchers to gain access to information that will immensely progress xenotransplantation.
The first heart transplantation from a genetically engineered pig was performed on January 7, 2022, in Baltimore, led by the University of Maryland School of Medicine surgeon-scientists. This surgery offered a new chance for a 57-year old patient, David Bennett, who suffered from a life threatening disease, causing him to be bedridden for eight weeks prior to the surgery. As well, the patient was not eligible for a human donor heart, due to a history of inconsistentently sticking to treatment plans. Facing end-stage heart failure, a Xenotransplantation was the only option left for Bennett. At the time of Bennett’s case, the FDA had not approved pig-heart transplants, but permitted this surgery for as the medical team stated, “compassionate use”.
“We are very encouraged by this finding, and it suggests that the genetically-modified pig heart and the experimental drug we used to prevent rejection worked effectively in tandem to demonstrate that xenotransplants can potentially save future lives,” said Muhammad M. Mohiuddin, MD, Professor of Surgery and Scientific/Program Director of the Cardiac Xenotransplantation Program at UMSOM.
While Bennett showed no signs of rejection for several weeks post op, he passed away two months after the procedure. Bennett’s family says that they are grateful for the extra time the surgery allowed them to have together, and are hopeful for the future of this medical field.
Serving as the only life saving solution, the Xenotransplantation served as a temporary extension rather than a permanent solution for Bennett. While doctors are devastated by the loss of David Bennett, this operation leads to saving the lives of many in the future. “We remain optimistic and plan on continuing our work in future clinical trials,” said Muhammad M. Mohiuddin, MD.
May, 2022 data from the Polycystic Kidney Disease Foundation
Xenotransplantations are far from being perfected, but at this time have the ability to offer unique opportunities for select individuals. “You can never know if the person is going to die catastrophically soon after the treatment – but you can’t proceed without taking the risk…As long as the individual understands the full range of risks, I think people should be able to consent to these radical experiments,” says Professor Julian Savulescu, Uehiro Chair in Practical Ethics at the University of Oxford.
While heart xenotransplantations have not produced long term life saving results yet, doctors see the future of these operations as groundbreaking tools in the future. Once more studies are conducted and perfected, xenotransplantation will be opened to a larger pool of patients. Xenotranspanations have the potential to significantly shorten the waiting time for patients on the donor list, ultimately offering a life-saving chance to the 100,000 people in the United States alone.